Most often, brain death is a consequence of increased ICP, which may be the result of a variety of reasons: metabolic, toxic, trauma (head injury), infectious, neoplastic and idiopathic (tumor). When the ICP reaches a level that is equal to or greater than the MABP, the blood flow circulation in the brain will arrest and the brain will die.
Determining brain death has become very important in modern medicine due to its role in saving lives through organ transplantation. In most countries, there are guidelines and a specific protocol for determining brain death. All protocols require the use of a medical device. Transcranial Doppler (TCD) is one of the most common medical devices used in the diagnosis of and as a support decision tool for brain death determination due to its ability to detect the unique effect of brain death on cerebral blood flow pattern.
In many cases, when utilizing TCD for a brain death diagnosis, the operator is required to examine anterior and posterior cerebral circulation thoroughly. (Each blood vessel is examined for at least 3 minutes and the entire examination length is at least 30 minutes.) If complete circulatory arrest exists, there are patterns of flow cessation, oscillating patterns with negative flow in the diastole (Fig. 1), and short systolic spikes (<50cm/sec) (Fig. 2).
Digi-Lite TCD and Brain Death
The Digi-Lite TCD is used as a diagnostic tool for complete cerebral circulatory arrest in many countries around the world due to its very high sensitivity (97%), specificity (100%), and state-of-the-art summary screen that provides complete data for anterior and posterior cerebral circulation.
The Digi-Lite TCD can be used at the patients’ bedside; is repeatable; cost- effective; noninvasive; and used without sedatives, drugs, or contrast agents that could harm the kidneys or other organs (and therefore prevent organ donation).

 Figure 1: “To and From” Waveform Pattern (oscillating patterns with negative flow in the diastole when ICP becomes higher than diastolic ABP [irreversible]).
Figure 1: “To and From” Waveform Pattern (oscillating patterns with negative flow in the diastole when ICP becomes higher than diastolic ABP [irreversible]). 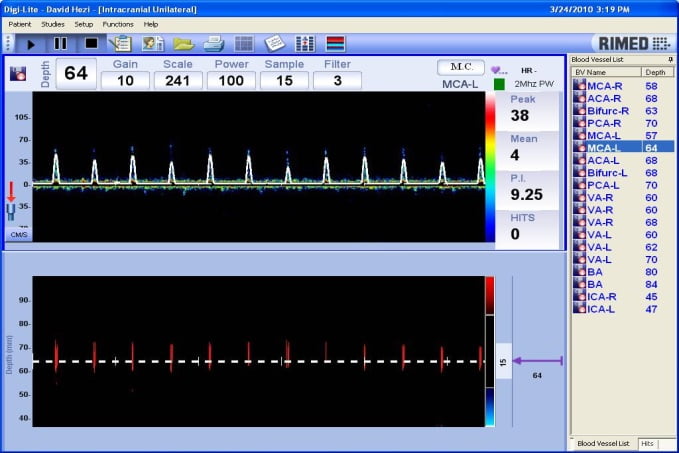 Figure 2: Short systolic spikes
Figure 2: Short systolic spikes  Figure 3: Digi-Lite’s summary screen displaying complete cerebral circulatory arrest
Figure 3: Digi-Lite’s summary screen displaying complete cerebral circulatory arrest 
